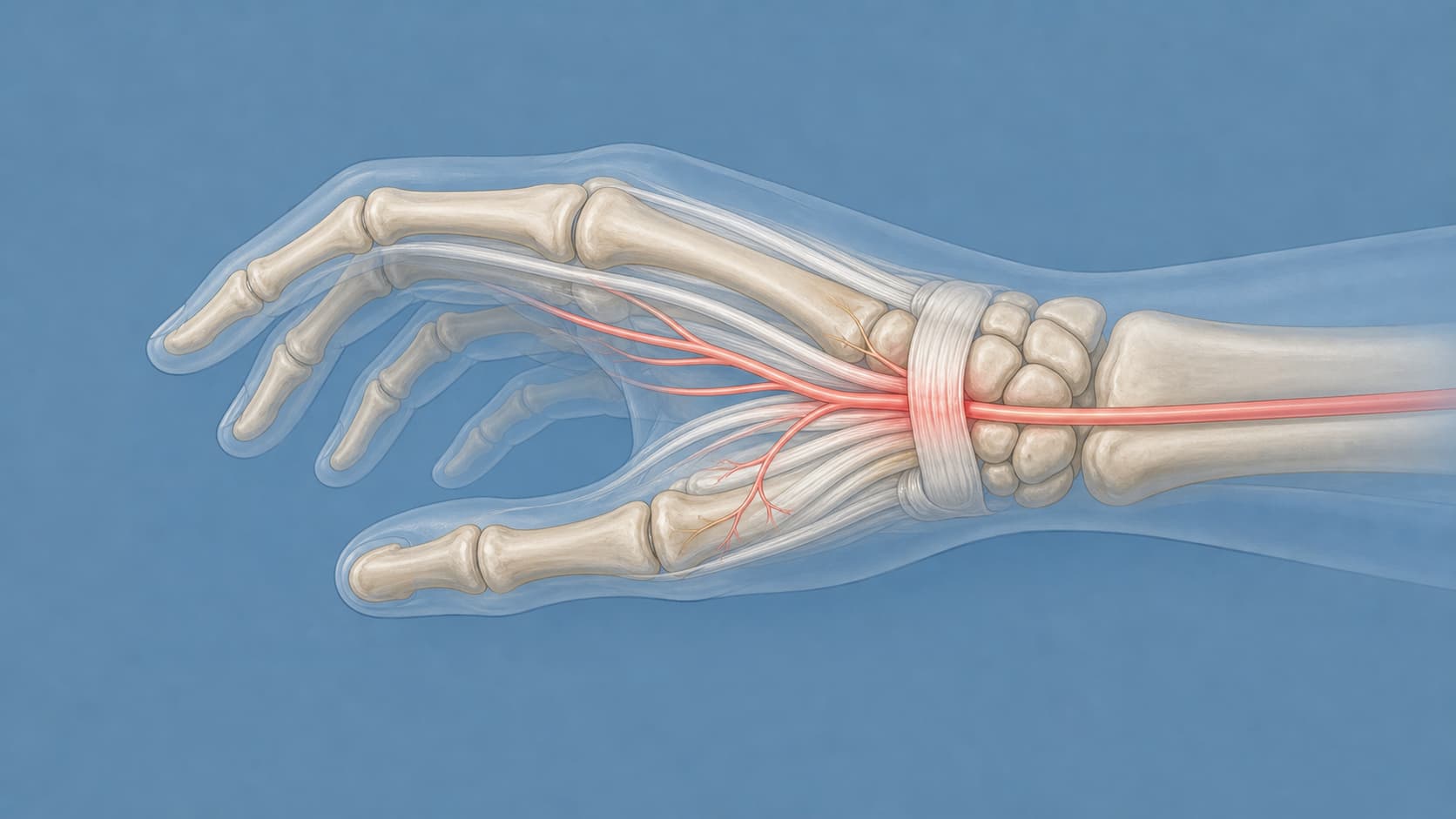
Anatomy of the carpal tunnel
The carpal tunnel is a narrow osseofibrous canal at the volar wrist. Its dorsal floor is formed by the carpal bones — arranged in a concave arch — and its volar roof by the transverse carpal ligament, also called the flexor retinaculum. Together these structures define a small, fixed-volume space through which ten structures must pass.
Nine of those structures are extrinsic finger flexor tendons: four flexor digitorum superficialis tendons, four flexor digitorum profundus tendons, and the flexor pollicis longus. The tenth is the median nerve, which lies superficial to the flexors and just deep to the retinaculum. Because canal volume is essentially fixed by the surrounding bones and ligament, any rise in tunnel pressure compresses the lowest pressure-tolerance structure inside it — the nerve.
One anatomical detail dominates the clinical picture: the palmar cutaneous branch of the median nerve arises proximal to the carpal tunnel and runs superficial to the flexor retinaculum, never entering the tunnel itself. This branch supplies the central palm. As a result, sensory loss in CTS classically affects the digits but spares the palm, a useful examination clue when the picture is ambiguous.
How carpal tunnel syndrome develops
Median nerve compression in the tunnel is the final common pathway for several mechanisms. Anything that raises tunnel pressure or reduces tunnel volume can drive it: synovial hypertrophy of the flexor sheath (most common in chronic repetitive use), fluid retention (pregnancy, hypothyroidism), space-occupying lesions, or wrist fractures and dislocations that distort the canal.
A second mechanism is the so-called double-crush phenomenon, first described by Upton and McComas. Proximal nerve irritation — for example from cervical radiculopathy at C6 or C7 — reduces axoplasmic flow and lowers the threshold for symptomatic compression at a more distal site. A patient with subclinical cervical disc disease may therefore declare CTS at the wrist long before the wrist itself is the dominant problem, and clinicians who only examine the wrist will miss the proximal driver.
Clinical features and presentation
Sensory symptoms appear first. Patients describe tingling, burning, or numbness in the thumb, index, middle, and the radial half of the ring finger. Symptoms are typically worst at night because flexed wrist postures during sleep raise tunnel pressure. The classic patient wakes at two or three in the morning with a dead, tingling hand and flicks the wrist vigorously to restore feeling — the so-called Flick sign, one of the more specific clinical features for CTS.
As the condition progresses, motor symptoms emerge. The recurrent motor branch of the median nerve supplies the thenar muscles (abductor pollicis brevis, opponens pollicis, and the superficial head of flexor pollicis brevis) and the first two lumbricals. Weakness presents as difficulty with opposition and a dropped grip. In severe, long-standing cases, thenar atrophy is visible — the eminence flattens out and the thumb rests in the plane of the palm rather than abducted in front of it. This end-stage presentation is the ape-hand deformity.
Functionally, fine prehension grips suffer first because they require the most discriminative sensation and the most precise thenar control. Tip-to-tip and tip-to-pad grips deteriorate before power grip does. Patients describe dropping small objects, struggling with buttons, or being unable to open jars they used to manage easily.
Examination and provocation tests
Bedside examination of suspected CTS rests on three classic provocation tests alongside a focused neurological examination of the upper limb. None of the tests is diagnostic on its own; the clinical picture, examination pattern, and (when available) nerve conduction studies make the diagnosis together.
Tinel’s sign
Tap firmly over the median nerve at the volar wrist crease, just radial to palmaris longus. Reproduction of paraesthesiae in the median distribution is positive. Tinel’s is sensitive but not highly specific — many median nerves are mildly mechanosensitive, and the test can produce a positive result without true CTS.
Phalen’s test
Have the patient hold the wrist in maximal flexion for sixty seconds. Reproduction of paraesthesiae or numbness in the median distribution is positive. The test relies on the fact that wrist flexion sharply raises pressure inside the tunnel.
Two-point discrimination
Two-point discrimination quantifies the loss of fine sensory acuity. It is more useful for tracking change over time than for making the initial diagnosis, but a two-point threshold above six millimetres in the median distribution suggests significant nerve dysfunction.
| Test | Sensitivity | Specificity | When it’s most useful |
|---|---|---|---|
| Tinel’s sign | ~50% | ~75% | Quick screen at the bedside |
| Phalen’s test | ~65% | ~75% | Quick screen; can be falsely negative in severe disease |
| Carpal compression test | ~65% | ~80% | Often more discriminative than Tinel’s or Phalen’s |
| Two-point discrimination | ~30% | ~95% | Tracking change over time, not initial diagnosis |
Differential diagnosis
Three differentials must be excluded in any patient referred with "carpal tunnel syndrome":
Pronator syndrome. Compression of the median nerve in the proximal forearm between the heads of pronator teres. Symptoms overlap with CTS but include forearm pain on resisted pronation and tenderness over the proximal forearm rather than the wrist. Crucially, the palm is involved because the palmar cutaneous branch is downstream of the compression.
Anterior interosseous nerve syndrome (AINS). A pure motor branch of the median nerve below the elbow. Patients cannot make an OK sign because flexor pollicis longus and the radial half of flexor digitorum profundus are weak. There are no sensory symptoms.
Cervical radiculopathy. C6 and C7 radiculopathies refer pain and paraesthesiae down the upper limb in patterns that overlap with CTS. Spurling’s test, neck range, and a careful dermatomal/myotomal examination distinguish them. Remember the double-crush mechanism — cervical and wrist pathology can coexist.
Conservative physiotherapy management
Most CTS responds to non-operative management, particularly in early disease. The aim is to lower internal carpal tunnel pressure, mobilise structures that have become adherent, and restore symptom-free function.
Splinting
A neutral wrist splint — zero degrees of flexion or extension — minimises internal carpal tunnel pressure and is the single conservative intervention with the strongest Cochrane support at four weeks. It is worn at night routinely and during symptomatic activities during the day. Avoid splinting in any flexion; even modest flexion sharply raises tunnel pressure.
Tendon-gliding exercises
Tendon-gliding exercises take the extrinsic flexors through their full excursion in differential ways: straight, hook, fist, table-top, and straight-fist positions. The goal is to promote independent tendon excursion and prevent adhesions inside the tunnel from limiting glide.
Median nerve gliding
Nerve gliding mobilises the median nerve through its envelope. Progressions move from gentle short-amplitude glides to longer-amplitude tensioners. The strict precaution is that nerve symptoms (tingling, electric sensation) must not be pushed through. Provoked symptoms are a stop signal — pushing on increases inflammation and makes the condition worse.
Carpal bone mobilisation
When carpal mobility is restricted, manual mobilisation of the carpal bones (especially the lunate and capitate) can improve tunnel volume.
Strength
During the irritable early phase, only gentle multiple-angle isometric muscle setting is permitted. Progressive resistance is introduced once nerve symptoms have settled and range is full and pain-free.
Surgical release and post-operative rehabilitation
Surgical release is reserved for cases that have failed an adequate trial of conservative management or that present with motor signs (thenar weakness, atrophy). The procedure is decompression of the canal by transection of the transverse carpal ligament, performed open or endoscopically.
Early post-operative phase
The major biomechanical risk after release is bowstringing of the extrinsic flexor tendons at the wrist, because the retinaculum that anchored them volarly has been cut. To prevent this, active wrist flexion past neutral must be avoided for the first ten days post-op, and up to three weeks in cases of extreme caution. The fingers, critically, are left free to move from day one to prevent tendon adhesions.
Pillar pain
Pillar pain is a well-described but poorly understood phenomenon: pain in the thenar and hypothenar eminences after release, thought to relate to flattening of the palmar arch when the retinaculum is cut. It typically resolves over three to six months and should be communicated as expected, not pathological.
Grip and pinch strength
A temporary fall in grip and pinch strength immediately post-op is normal because transection of the retinaculum alters the length-tension relationship of the thenar muscles whose anchor it provided. Strength typically returns over three to six months as the muscles adapt.
Sensory recovery
Sensory modalities return in a predictable order as the median nerve recovers: light touch first, then sharp/dull discrimination, then two-point discrimination. Severe long-standing pre-operative compression carries a higher risk of incomplete sensory recovery.
Common questions
Real questions students and clinicians ask.
- Does typing on a keyboard cause carpal tunnel syndrome?
- AThe evidence is weaker than the popular belief. Sustained gripping, repetitive flexion, and exposure to vibration are more strongly linked than ordinary keyboard typing. Occupations like assembly-line work, plumbing, and tile-laying carry higher risk than office desk work.
- How long should I trial conservative treatment before considering surgery?
- AMost guidelines suggest a structured 4 to 12-week trial of splinting and physio. Earlier surgical referral is reasonable in patients with motor signs (thenar atrophy, weakness) because waiting risks incomplete recovery.
- Can carpal tunnel syndrome resolve on its own?
- AMild CTS, especially when triggered by a transient cause like pregnancy, can settle without intervention as the underlying driver resolves. Established disease with motor signs rarely resolves spontaneously.
- Why does my hand feel worse at night?
- AWrist flexion during sleep raises pressure inside the carpal tunnel. Most patients sleep with the wrist gently flexed for hours, which compresses the median nerve. A neutral night splint usually settles this within a week or two.
Quick reference
The 32 questions below mirror our flashcard deck. Read them as a self-check, or open the deck for full spaced-repetition study.
- What anatomical structure forms the dorsal boundary of the carpal tunnel?
- ACarpal bones.
- What anatomical structure forms the volar boundary of the carpal tunnel?
- ATransverse carpal ligament (flexor retinaculum).
- Which specific nerve is compressed in Carpal Tunnel Syndrome (CTS)?
- AMedian nerve.
- What structures accompany the median nerve through the carpal tunnel?
- ANine extrinsic finger flexor tendons.
- Why is the palm of the hand usually spared from sensory loss in CTS?
- AThe palmar cutaneous branch of the median nerve arises proximal to the carpal tunnel.
- What classic nocturnal symptom behavior is highly indicative of CTS?
- AWaking with numbness/pain and vigorously flicking the wrist for relief (Flick sign).
- Which specific intrinsic hand muscles weaken and atrophy in late-stage CTS?
- AThenar muscles and the first two lumbricals
- What visible hand deformity is caused by severe median nerve compression and thenar atrophy?
- AApe hand deformity.
- Which intrinsic muscle of the thumb often develops tightness in CTS due to opposing muscle weakness?
- AAdductor pollicis.
- What systemic condition involving transient water retention is a common non-traumatic cause of CTS?
- APregnancy.
- What provocation test involves tapping the median nerve at the volar wrist?
- ATinel's sign.
- What provocation test involves sustained maximal wrist flexion to compress the median nerve?
- APhalen's test.
- What sensory test is typically used to quantify discriminative sensation loss in CTS?
- ATwo-point discrimination test.
- What two forearm conditions must be differentiated from CTS because they also cause median nerve symptoms?
- APronator syndrome and anterior interosseous nerve syndrome (AINS).
- What mechanism explains why proximal nerve irritation (e.g., cervical radiculopathy) increases susceptibility to distal compression?
- ADouble crush syndrome.
- What three combinations of wrist motions are considered the most mechanically aggravating for CTS?
- ASustained flexion, ulnar deviation, and repetitive flexion/extension combined with gripping.
- What functional prehension grips are most impaired in CTS due to loss of fine neuromuscular control?
- ATip-to-tip and tip-to-pad grips
- What is the initial non-operative splinting angle for CTS?
- ANeutral (0 degrees) to minimize internal carpal tunnel pressure.
- Which hand joints require manual mobilization if restricted in a patient with CTS?
- ACarpal bones (to increase carpal tunnel space).
- What is the primary physiological goal of performing tendon-gliding exercises in CTS?
- ATo promote mobility of the extrinsic tendons and prevent adhesion formation.
- What is the strict precaution when progressing through median nerve gliding positions?
- AStop progressing the moment symptoms (e.g., tingling) are provoked; do not push through nerve pain.
- What is the only type of resistance exercise permitted in the initial early stages of CTS rehab?
- AGentle multiple-angle muscle-setting (isometric) exercises.
- What conservative intervention is most strongly supported by Cochrane reviews for alleviating CTS symptoms at 4 weeks?
- AA hand brace (splint).
- What anatomical structure is surgically transected to decompress the carpal tunnel?
- ATransverse carpal ligament.
- What biomechanical complication is a primary risk immediately following surgical release of the flexor retinaculum?
- ABowstringing of the extrinsic flexor tendons at the wrist.
- What specific active wrist motion must be strictly avoided during the early post-op phase of a CTS release?
- AActive wrist flexion past neutral (prevents flexor tendon bowstringing).
- For how long post-operatively must a patient avoid active wrist flexion past neutral?
- AFor the first 10 days (and up to 3 weeks for extreme caution).
- Are the fingers immobilized during the initial 7-10 days after a carpal tunnel release?
- ANo, fingers are left free to move to prevent tendon adhesions.
- What is 'pillar pain' following CTS surgery?
- APain in the thenar and hypothenar eminences caused by the surgical release and flattening of the palmar arch.
- What is the expected timeline for the resolution of 'pillar pain' and post-op grip weakness?
- A3 to 6 months
- What physiological change explains the temporary decrease in grip and pinch strength immediately after CTS surgery?
- AAltered length-tension relationship of the thenar muscles due to the transection of their anchor point (transverse carpal ligament).
- Which sensory modality typically returns first as neurological symptoms resolve post-surgery?
- ALight touch.
References
- American Academy of Orthopaedic Surgeons (2024). Management of Carpal Tunnel Syndrome: Evidence-Based Clinical Practice Guideline. AAOS.
- Page MJ, Massy-Westropp N, O'Connor D, Pitt V (2012). Splinting for carpal tunnel syndrome. Cochrane Database of Systematic Reviews. doi:10.1002/14651858.CD010003
- Magee DJ (2014). Orthopedic Physical Assessment, 6th edition. Saunders.
- Upton ARM, McComas AJ (1973). The double crush in nerve entrapment syndromes. The Lancet. doi:10.1016/S0140-6736(73)92193-7
- MacDermid JC, Wessel J (2004). Clinical diagnosis of carpal tunnel syndrome: a systematic review. Journal of Hand Therapy. doi:10.1197/j.jht.2004.02.015